Stoma Care
Greater care is required during the first week the tube is in place, as the surgery has just been performed. Your stoma (the feeding tube site) is, essentially, a stab wound that you don’t ever want to fully heal because that would mean that the stoma is closed and you’ll need another PEG surgery. The area around the wound must be kept thoroughly clean and covered with clean gauze. During this period of time, the tube may occasionally pull away from the abdominal wall, resulting in leakage around the insertion site. Leakage may also occur if the stoma site becomes enlarged.
Healthy stomas for button and G-tube:
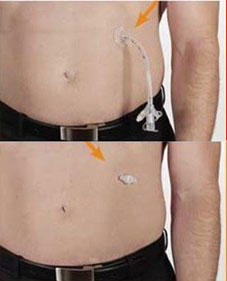 Chronic leakage around the site is NOT normal. If the stoma is oozing blood, food, stomach acids, or any other substance, then you need to see your GI or visit the ER immediately.
Chronic leakage around the site is NOT normal. If the stoma is oozing blood, food, stomach acids, or any other substance, then you need to see your GI or visit the ER immediately.
The tube is marked at the point where it should be level with the incision and should be checked regularly to make sure it is still properly in place. Excessive tension on the tube may result in pressure necrosis (death of an area of tissue) of the interior abdominal wall. Excessive tension may also cause the tube to be pulled out prematurely.
Should the tube accidentally come out, the original tube–or a replacement–needs to be placed back in the stoma as soon as possible or the incision will begin to heal, and new surgery may be required. Stomas could begin to close up in less than two hours. It behooves you to have a spare, balloon tube (or a Foley Catheter, which also has a balloon) at home in case your tube comes out and you don’t have immediate access to an ER.
Along these lines, you should be familiar with how to replace your own tube. After your first PEG surgery, ask the surgeon for specific instructions for changing the tube. Or, at your next GI visit for a regular tube change, watch your doctor carefully to see how it’s done. Even better, ask your doctor to let you do some of the procedures so you can boost your confidence.
Daily showers should be sufficient to keep the stoma site clean after it has healed from the initial surgery. The site may have occasional ‘crustiness’ or granulation around the edges. This is normal. The body is simply attempting to repair slight pulls, tears or minor infections. The granulation should just be gently washed off.
On the other hand, if you see unnaturally swollen, red, lumpy, moist tissue or flesh around the stoma site, then it is most likely what’s known as hypergranulation tissue. This tissue could also exude yellow, sticky pus. It may be painful, bleed easy, and prevent your stoma from healing the way it should. Hypergranulation can occur for no apparent reason (friction, moisture or irritation may be contributing factors), especially during the first three months after the tube has been placed.
There are different methods for dealing with hypergranulation tissue. Initially, you should keep the site clean and dry in the hope that it will heal by itself. If this doesn’t work, silver nitrate may be an option. Silver nitrate is a caustic substance that burns the offending tissue. It will turn black as a result, scab up and eventually fall off. Note: you should spread petroleum jelly around the stoma before administering silver nitrate because it is extremely painful when it touches the skin. Other ointments have also proven to be effective at getting rid of hypergranulation. Creams intended for ear infections or skin issues (such as Kenacomb) may heal the site. Some G-tube patients report that 4-5 administrations of Kenacomb per day for five days clear up their hypergranulation. As a last resort, some doctors could choose to surgically remove the hypergranulation tissue. Wound care is extremely important after such a procedure to avoid infection or a reoccurrence.
You should regularly rotate your G tube, beginning a few days after initial placement. This makes sure the tissue and skin around the area haven’t stuck to the tube and will give you a good healthy stoma. It’s recommended that you rotate the tube at least a quarter turn once a day. The best time is probably right after you bathe. If the tube feels tight and is difficult to turn, be sure not to force it. Make sure there is a little space in and out for the tube. If it’s too tight against the skin, slide the g-tube bumper up slightly. If your tube is held in place by a balloon, check to see if there is enough water in the balloon (see below). It could be that the balloon has burst or eroded–this necessitates a tube change. If the feeding tube freely moves in and out and the balloon appears undamaged, try lubricating the stoma with a little water-based lubricant. If you don’t have lube, you could try using vegetable oil. Vaseline, or other petroleum-type lubricants, erode the plastic in the feeding tube over time so you should avoid using these. Once the tube is lubricated, try rotating it again. Use as much gentle force as you’re comfortable with but note any pain or discomfort. Don’t panic if your tube won’t rotate. Stomas commonly get tight due to bloating, recent tube placement, or tube changes. However, if you’re unable to rotate your tube more than a few days, ask for medical advice.
How to check the water in your balloon.
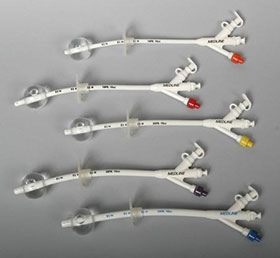 Your tube should have an access port for the balloon (the colored port on the tubes pictured at right). Insert a syringe into this port (the 60 cc syringe you use for feeding may have a special luer adapter for this purpose). Gently draw back on the syringe while making sure it is firmly attached to the port. Clear water should be drawn into the syringe–the same amount that was put into the balloon when placed. If the water is not clear, or there isn’t enough, or you’re not able to get any at all, then there is a problem with the balloon and you need to get your tube changed. If the water is fine, then you can slowly push it back into the balloon.
Your tube should have an access port for the balloon (the colored port on the tubes pictured at right). Insert a syringe into this port (the 60 cc syringe you use for feeding may have a special luer adapter for this purpose). Gently draw back on the syringe while making sure it is firmly attached to the port. Clear water should be drawn into the syringe–the same amount that was put into the balloon when placed. If the water is not clear, or there isn’t enough, or you’re not able to get any at all, then there is a problem with the balloon and you need to get your tube changed. If the water is fine, then you can slowly push it back into the balloon.
Tube Care
To keep the tube clean and unobstructed, you should flush the tube with clear water before and after feedings, or after medications have been administered through the tube. After the tube is placed, you should consult a registered dietitian or a nurse who specializes in nutrition to determine your nutritional needs, the number of calories, protein, and fluids that will be necessary, as well as the most appropriate nutritional formula and how much of that formula will be needed each day. Nutritional products designed for tube feeding are formulated to provide all the nutrients you’ll require including proteins, carbohydrates, vitamins, and minerals. Some even contain dietary fiber and other non-nutritional elements. If you choose to blend food for your meals, you should consult your doctor or nutritionist to make sure you are meeting your nutritional needs.
When eating through a tube, it is imperative that you, or your caregiver thoroughly wash your hands with soap and water before preparing formula or having contact with the PEG system–much as you’ve always had to wash your hands before eating. The tube should be checked for patency, and the formula administered at room temperature. You should be upright, no less than thirty degrees, to minimize the risk of regurgitation and aspiration, and you should be kept upright for thirty to sixty minutes after feeding. In some cases, to prevent complications like abdominal cramping, nausea and vomiting, gastric distension, diarrhea, or aspiration, food should be infused slowly. It may take more than an hour to administer one feeding session, as the drip mechanism is kept at very slow settings. Sometimes continuous feeding is preferable. With this method, a feeding pump is set up and connected to the PEG tube. The formula is infused over a prescribed period of time into the patient. The risk for aspiration is decreased because less formula is given during a more prolonged period of infusion. Using an attached bag system to contain the liquid diet for feeding is a secondary method by which food is allowed to drip slowly into the tube though “gravity feeding.” With this technique, there is greater freedom in that feedings can be done anywhere, at any interval, and medications may be administered through the PEG tube utilizing this method. Under the drip-feeding method, feedings are usually performed every four to six hours. Clogging of tubes is regularly reported, especially in small-bore tubes. Tubes should be flushed with water before and after feeding during intermittent delivery, and every 4 to 8 hours during continuous feeding. This is done with a syringe full of water which is attached directly to the tube. Multiple flushings with the syringe will ensure a free-flowing system. The patient may experience bloating either before or after feeding. If this occurs, the stomach and intestinal tract should be decompressed. Removing the adapter feeding cap from the tube and allowing the PEG to be open to air can easily accomplish this. Encouraging the patient to cough will also facilitate decompression.
The lifespan of the feeding tube is about six months. When the tubing begins to wear, it may pull away from the stomach wall and cause leakage near the insertion point. The replacement process is relatively simple and usually does not involve another endoscopic procedure. Typically, the tubing is merely pulled out through the stomach site and then replaced with a new catheter.
Complications to this therapy may occur, but the likelihood is slight, with only a one percent chance of major problems (gastric hemorrhage, peristomal leakage) and an eight percent chance of minor ones (infection, stomal leaks, tube extrusion or migration, aspiration and fistula formation). Aspiration is perhaps the most common complication related to tube feeding. This occurs when food is actually inhaled into the lungs. Aspiration can lead to pneumonia, but if the patient is kept upright during feeding, the likelihood of developing this complication can be greatly minimized.
Clogs
The best way to deal with clogs in the feeding tube is to not get a clog in the first place. This is why it is always important to flush the tube with plenty of water before and after feeding. Also, make sure all medications are completely crushed. Tubies have frequent problems with reflux medicine like Prevacid or Nexium getting stuck in the tube. These meds are normally tiny balls packed in capsules and the balls often clump together in narrow passages like feeding tubes. The best way to take this type of medication is to suspend the tiny balls in something thicker than water. Applesauce works very well for this and can be pushed through the tube fairly easily. Another preventative measure for clogs is to make sure your food is well blended. Commercial formulas are designed to easily flow through feeding tubes, however blended meals need to be blended with a high-end blender, like a Vitamix or Blendtec, or strained before they are put into the tube (see the section on Homemade Tube Nutrition).
If a clog does occur, there are simple steps you can take to try to clear out the obstruction. The first step is to pull the clog out. This may seem simple and obvious, yet when many tubies are confronted with a clog, their instinct is to just push harder to get the offending item in. This may just exacerbate the issue or lead to an explosive mess. The simplest solution is to take out your syringe, take a few deep breaths, push the plunger all the way into the syringe, reattach it to the feeding tube, and pull the plunger out to force the clog out the way it came.
Another way to clear clogs is to use warm water. Many tubies are firm believers in the idea that Coke, or other types of carbonated beverages, is the ideal way to remove a clog. In fact, there is no evidence that Coke is any more effective than water. While Coke has worked for some, it is just as likely that their clog would have been removed with time and water. Allowing the clog to soak in warm water gets it nice and wet and soft around the edges. The best way to do it is to load the syringe up with water, attach it to the tube and gently push it until it meets the clog. Next, lightly push and pull on the syringe and see if the clog moves at all. Be patient with the clog. After gently pushing and pulling with warm water around the clog, it should come lose and you can push it the rest of the way into your stomach. If the clog refuses to go in any further, but you can pull it out, make sure to draw it out completely into the syringe. Then you can clamp your tube, detach the syringe, and get rid of the clog.
Patience is key here. It could take 20 minutes to move the clog, but dealing with it at home is preferable to going to the ER. Just keep the warm water against the clog with a syringe and gently try pushing and pulling on it every few minutes. Eventually (hopefully) the clog will get mushy enough to move through the tube.
While Coke, or other carbonated drinks, have little or no effect on clogs, there are other liquids that may help break down the clog. Instead of warm water you can try meat tenderizer, papaya juice, mango juice, pineapple juice, or kiwi juice. There is also a product available online called Clog Zapper that is specifically made to unclog feeding tubes (one of the main ingredients is also found in meat tenderizer and papaya juice). All these will also take time (about 10-20 minutes) to work but the enzymes in these products should soften most clogs enough for you to clear them.
We hesitate to recommend this, but another possible way to get rid of clogs is to stick something down the tube. Be smart about this. Nothing unsanitary, or too long, or damaging to the tube. Actually, there are commercial tools called Enteral Feeding Tube DeCloggers that are designed to remove clogs, however they are for single-use only and are fairly expensive (around $25 for one). Other tubies have had success with knitting needles, bamboo skewers or pipe cleaners. Before using anything, be sure to measure the length of your feeding tube to prevent pushing the tool in too far.
If all else fails, then you should make a trip to the ER or contact your GI to get your feeding tube changed immediately.
Clogs are common for everyone who tube feeds, whether they blend their meals, or just eat formula. Every tubie has their humorous clog stories. A survey of a couple tube feeding support groups unearthed these gems:
- One tubie said that, “My feeding tube got clogged with riboflavin (which turns cement-like if you don’t mix it with enough water) and when I finally pushed hard enough to get it to unclog, it went, well, everywhere :)”
- Another sprayed a blend across the room and into her husband’s guitar.
- Rachel shared this incident: “My husband was feeding my son in the waiting room at an appointment while I registered him. I walk back over to them and my husband says, ‘Can you take care of that?’ while pointing at another child in a stroller near us. There was a spray of [blended diet (BD)] all over the back of the stroller. As an added bonus, the family was not native English speakers.”
- Rebecca is another caregiver to a tubie: “Our 21 year old son has “girly” posters on the ceiling in his room. I was trying to get his j-tube unclogged (formula) and sprayed a group of his beach beauties. Not quite the spray tan you hear of….”
- Jen said, “Our first month of BD was at an [ICU]. The first day of the diet, I ended up spraying not just any ceiling but the room’s popcorn ceiling. It wasn’t an easy explanation to make about why a green substance was on the ceiling!”
- Lindsey had a couple stories: “I was in Target and the pump kept beeping…I finally took pump and bag out of the backpack to inspect. I squeezed the bag too hard and the top flew off from the pressure and covered me including face and hair, my child and the contents of my cart…”
The most important thing, when dealing with a clog, is to have the right attitude. You’re not alone. All tubies have been there! Laugh it off, talk about it openly with the people around you, and share it on one of the tubefeeding forums with people who understand.
 Feeding through a tube requires a catheter-tip syringe. This syringe has a tapered tip made for fitting into a catheter opening, extension set, or feed port (typical syringe with blue luer adapter pictured at right). There are also slip-tip syringes with a narrower tip offset from the barrel of the syringe (below, at left). These could come in handy if you want to mix up your medications inside the syringe. A third type is the Luer-lock syringe (below right). These syringes have a special tip designed to mate with a particular medicine port. The two sides lock together with a quarter-twist. Another example of a Luer-lock fitting is the button-end of the extension set.
Feeding through a tube requires a catheter-tip syringe. This syringe has a tapered tip made for fitting into a catheter opening, extension set, or feed port (typical syringe with blue luer adapter pictured at right). There are also slip-tip syringes with a narrower tip offset from the barrel of the syringe (below, at left). These could come in handy if you want to mix up your medications inside the syringe. A third type is the Luer-lock syringe (below right). These syringes have a special tip designed to mate with a particular medicine port. The two sides lock together with a quarter-twist. Another example of a Luer-lock fitting is the button-end of the extension set. Syringes need to be washed well after use (just like you’d wash your dishes after eating). The plunger on most syringes has a rubber tip. After repeated use, the rubber deteriorates and expands, making it much harder to push through the barrel. For this reason, syringes can’t really be used more than about a week before they need to be replaced. An alternative to the rubber-tipped plunger is the o-ring syringe. O-ring syringes (also known as ‘squirrel syringes’) have plungers with silicone o-rings on the end. They are a bit more expensive but can last much longer than other syringes. Many tubies have used the same o-ring syringe over a year–just washing after each use. These syringes are available from Real Food Blends or try asking your local veterinarian–they’re normally used to feed small animals.
Syringes need to be washed well after use (just like you’d wash your dishes after eating). The plunger on most syringes has a rubber tip. After repeated use, the rubber deteriorates and expands, making it much harder to push through the barrel. For this reason, syringes can’t really be used more than about a week before they need to be replaced. An alternative to the rubber-tipped plunger is the o-ring syringe. O-ring syringes (also known as ‘squirrel syringes’) have plungers with silicone o-rings on the end. They are a bit more expensive but can last much longer than other syringes. Many tubies have used the same o-ring syringe over a year–just washing after each use. These syringes are available from Real Food Blends or try asking your local veterinarian–they’re normally used to feed small animals.Extension sets (used if you have a button) can be cared for much like syringes. They probably won’t get thoroughly cleaned in the dishwasher because it’s hard to flush water all the way through them. The best way to clean them is to run hot, soapy water–or just hot water–through them (you can push it through with a syringe), rinse them out, and air-dry. You can also soak them in a vinegar solution (50% vinegar and 50% water will do the trick) to kill most germs. Extension sets should last from one week to one month if they’re well cared for.
Feeding bags, used with pumps, are meant to be one-time-use only, but they can be washed and reused if necessary. As with syringes and extension sets, hand wash bags in hot, soapy water and/or soak them in a vinegar solution. Thorough cleaning is essential because formula has been sitting in the bag for a long period of time.




