Proper nutrition is a vital part of cancer treatment. It can be extremely difficult to not only get the essential nutrients needed for healing of your body and maintenance of your immune system, but also to maintaining body weight, and the percentage of lean body mass (muscles) during chemotherapy and radiation treatments for oral cancer. A healthy diet–including proteins, fats, vegetables, carbohydrates and AMPLE HYDRATION–will make your cancer treatment easier, and your recovery time shorter. Make certain you know where to go to get approved nutrition guidelines. Be sure to consult your doctor or nutritionist about vitamins, minerals, antioxidants, phytonutrients, probiotics and prebiotics. The pages in this section of the OCF web site are a good starting point. There are many aspects of your treatment that will certainly be out of your control. It is difficult to feel like a spectator in the process of becoming cancer free, and not an active participant in your return to full health. Good nutrition is something that you will have control over and will contribute to your rapid return to wellness in a significant way.
As you progress through treatments, you may develop difficulty chewing and swallowing solid food. The treatments can cause mucositis sores in your mouth, radically alter the amount of saliva you have that aids swallowing, as well as destroy temporarily your ability to taste things. It may become necessary to blend your meals and drink them orally. We provide tips for blending your food, as well as resources to find balanced recipe ideas. If things get really bad and even liquid nutrition taken orally is not keeping you properly nourished, your body weight begins to drop radically, and this must be stopped. Your doctors will set a limit on the amount of weight and lean body mass they are comfortable with you losing, and reaching that point, you will need to think about getting a feeding tube. This can be a frightening step for cancer patients. Many patients have bad connotations associated with feeding tubes, but they are simply another tool you can use to get the nutrition you need to beat your cancer. Discussions about this with your treatment team, combined with a physical assessment of your physical condition for optimum tolerance of treatments and healing, will at some point be necessary.
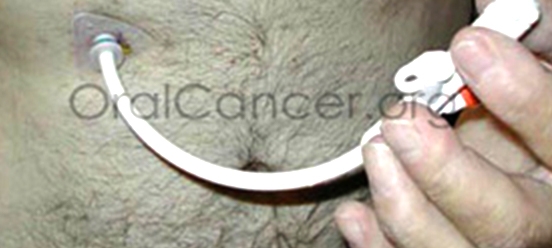
Feeding tubes come in lots of different configurations and designs depending on if they are going to be used for very short periods like a month, or for a longer period. In the links above we will discuss all the different types of tubes for different situations such as NG, NJ, J, GJ, and G tubes. Many people get nervous about the procedure for inserting a tube. The procedure is common, and your gastroenterologist that is going to put it in has done many of them. It is a very short and simple surgical procedure, done as an outpatient. The links above will walk you through the process for tube insertion so that you are knowledgeable and not anxious about it.
Once you begin using your feeding tube, like anything new, there are some basic techniques that you will have to learn to live with yours comfortably until its eventual removal. Everything from the volume and temperature of your feeds, to your body position while feeding will affect how your body reacts to the food. Each person is slightly different, and at the beginning there will be some experimentation of what works best for you. There are different ways of feeding such as bolus feeding (using a large syringe to put food in your tube), gravity feeds (using a drip bag) or utilizing a pump. You may need to regularly vent and/or aspirate your tube, and you will need to flush and clean out your tube every time you use it. While your treatment team will see that you know this, we will cover it as well, and provide you with options and work-arounds when you find issues with it all. The OCF patient support group which is anonymous and free on this web site, has lots of people in it that are going through the same things you are. Joining the group will allow you to exchange ideas with others who are survivors, or just ahead of you on the treatment path. They are a wealth of knowledge, and we highly recommend that you come join the group as you go through your treatment process. Feeding is only one of the many topics being talked about every day of the week in the support group. If you have not already discovered it you can go to it direct through this link:
There are many options out there for commercially available liquid nutrition. Everything from Carnation Instant Breakfast, Boost, Ensure, to formulas that are only available via prescription like Jevity. In the short run these are adequate to get you through things. There are more elemental formulas, or formulas that use real foods you are accustomed to like fish and vegetables that have been liquefied available from companies like Real Food Blends. You should choose the right formula after looking at the ingredients and talking with your doctor or nutritionist.
The page in the links above also discuss possible complications that arise form tube feeding include unexplained pain around the tube, infections at the tube site, hypergranulation tissue, clogs in the tube, and burst bubbles or holes in the tube. You may need to check water in your balloon (if you have one) or change your tube yourself at home. Also, your equipment (for instance, your feeding pump) may malfunction. In addition, you need to be aware that switching to an all-liquid diet through your tube will likely affect your GI tract especially in the beginning as your body adjusts to this new process.
Finally, the information in this part of the web site is written for both patients and their caregivers. Spouses and other family members may be in the position of caring for tube feeders who are temporarily unable to feed themselves. They need to be familiar with all the information here as well. While all new this is not a difficult process, and you will rapidly become accustomed to the ins and outs of working through all the different components of feedings. Just remember that becoming a student of good nutrition, and maximizing your mealtimes during this difficult treatment process means that you can contribute to your own health during treatments and during the healing time afterwards.