Many who are following this story are far removed from neck surgeries, and even those of us that have been through them really are not versed on what actually happens as we experience them under the dream state of anesthesia. While I explain neck dissections to patients several times a week along with bone grafting, flaps, harvesting bone from secondary sites to rebuild anatomical structures lost to cancers and so much more in minute detail, I’ve never actually been part of it all. My knowledge about trauma is certainly real world, but about surgery it’s totally didactic. Lectures, scientific papers, and more sources have left me more than literate in it all. I know what/where/why of all the internal structures, and I completely understand the process technically; but actually being there is a whole “nuther” thing. I think most of us think of surgery the way it has been produced for us on TV. Well news flash…especially in an environment without modern equipment that works right, with a shortage of supplies from hemostats to the right suture material, to power going off in the middle of a complex procedure with routine, and beginning the process without scans and x-rays to prep you for what’s there… it’s wildly different. And the blood is not neat and tidy, but occasionally pooled in pockets you formed on each side of the patients neck when you draped them.
I really don’t want to make this post about science so much, but someone did ask about these huge growths we are removing, and I will just quickly tell you what these are. These are thyroid goiters. We don’t see this stuff in the states, because when it happens (as very small nodules and growths) it gets dealt with early, not after ten years of growth, and it just isn’t as common an occurrence. In the third world such as where we operated, one absent of much available medicine, a population that makes 2 dollars a day if anything; in this environment people will live with a growing mass for a decade or more allowing it to become these giant things you are seeing in the images. Ironically, some of this could be circumvented if BASIC things were available to them. One of the most common cause is a lack of iodine in the diet of these people. We in the first world / western, learned the consequences resulting from a lack of it, and we routinely buy items that have had it added, such as table salt and other common foods that are artificially iodized – without even thinking about it – because we need this in our diets and have found simple mechanisms around the issue to obtain it. Unlike vitamin D which our bodies can make from just sunshine, this necessary nutrient is not made by our bodies. In Africa a small source of it is a common banana, but one of those little yellow bits of delight in the great natural packaging has only about 2% of the daily recommended intake. In first world eastern cultures, the eating of seaweed in salads, and as a ubiquitous sushi component, eating just a quarter ounce will give you 3000 times the required daily value. These enlarged thyroids can be benign or malignant, but even if benign, when of the sizes you see in my posts, they compress the trachea compromising breathing, compress the esophagus, compromising the ability to swallow, and when a goiter extends down into the chest, blood returning from the neck and head can be partially obstructed, causing neck veins to bulge, causing a cascade of additional problems. So they compromise life in serious ways. OK so much for the lesson part of all this.
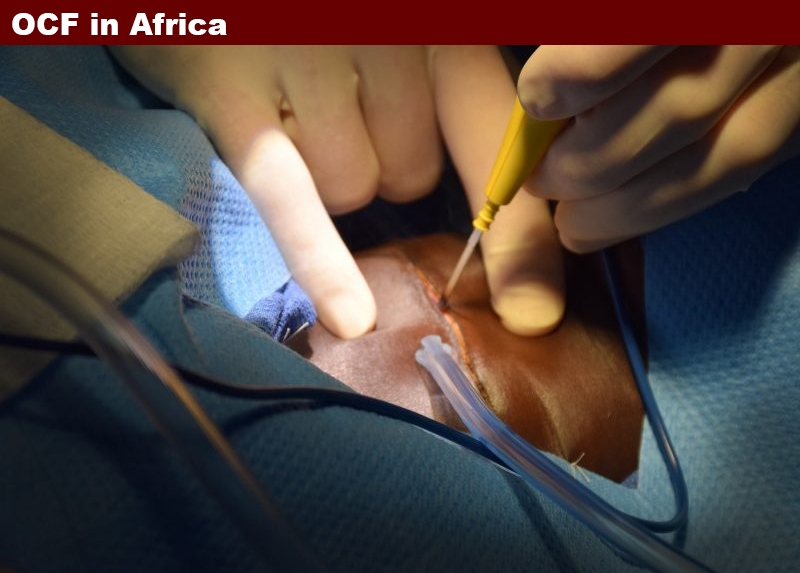
While we all think in terms of scalpels and the sharp blades on them as being the primary tool of surgery, there is a completely different approach, which has significant advantages in certain environments. It is electro surgery, a tool commonly known as a “bovie.” You can Google it if you want to know the details, but in some of the images you will see it in one of its applications, the cutting of tissue. The advantage is that while cutting, it is also cauterizing the cut as it goes… meaning not so much bleeding. Pretty cool. Mark is clearly the master of the bovie, though I suspect a scalpel is an equally routine part of his world as well. With our first anesthetized patient on the table, having skillfully been pre sedated by our volunteer nurse anesthetists, and now in the hands of another stationed at the head of our table; who with outdated monitors and equipment is regulating and responding to every change in the patient’s breathing, heart rate and more, making the necessary adjustments controlling their sedation; Mark draws a clean line across the center of the growth. Imagine the equator on the earth…through this demarcation we will enter the patient’s neck, right above the center of the mass and gradually begin separating the surrounding tissues away from it. With the six inch plus incision made using the bovie, and not a drop of blood on the the patients neck yet, I’m kinda amazed. Suction in hand ready to follow his cut, I realize I’m holding a device that at this juncture is completely unnecessary. I mean this is surgery right?….I’m ready for blood!
Mark places a pair of small retractors (they get really big as we progress) under the edge of the freshly incised skin, and passing them off to me I use them to pull the superficial tissues directly upward. Like he is using a small paint brush, he begins to separate the underlying mass and surrounding structures from the superficial tissues above and around it. His motions are more like a small paint brush on a canvas than a cutting instrument, and the bovie effortlessly is guided around the circumference of the mass creating a deeper and deeper entrance into our patient’s neck exposing the large mass. (When I say effortlessly, remember I am watching someone who has thousands of surgeries of greater complexity under his belt). Naively, I’m thinking to myself this is going to be a pretty simple process. WRONG, we just haven’t gotten to the interesting part yet, even though we are pretty far down around the sides of the mass by now. Throughout all this Mark is generously describing everything that is transpiring in detail; what we are doing, why, and what’s next. Helping me reposition the retractors, suction where needed, reminding me far too often to keep my hands out of his field of view, he is an instructor of not just detail and procedure, but possessing the patience born of hundreds of first year surgical residents in his portfolio of experiences…. all making the same mistakes which he clearly anticipates, and calmly corrects. More on this later in the next post because this is a really important point.
So my education advances rapidly, and I am now beginning to get ahead of him with his needs. I mean I’m retracting the tissue to keep his field of vision clear with both hands, and learning (uncomfortably) that this involves some hand, arm, and upper body yoga poses to accomplish; keeping everything where it is supposed to be, and my hands out of his field of vision….. Simultaneously, I hold two retractors under tension, a hemostat that is clamping off an early blood vessel that we needed to cut through, and some forceps that are being routinely used to lift and separate tissues which can also be touched with the bovie to send an electrical current down them to cauterize something like a small blood vessel captured between their tips. It’s a handful (literally), and to the inexperienced, keeping it all in place and keeping the tissues under tension with the retractors as a few minutes turns into 30, can be numbing. My neck muscles are giving out, my back hurts, my hands want to cramp, but addressing any of those things is not an option.
Mark has a cool technique of pushing a long pair of hemostats through the tissue and then out of it an inch or more away. Then he spreads them open, creating a taut area of tissue; then with the bovie a cut is made down the center. He repeats this around and around the mass. There is a regularity and rhythm to it, exposing more and more of the goiter as it is separated from the surrounding tissue.
We are now deep enough after about 40 minutes to get to the place where we are starting to really run into lots of blood supply. All growths and tumors many of us are so familiar with, create through angiogenesis, a nutrient /blood supply that allows them to grow and prosper. As we encounter each one of many vessels, Mark clamps it twice and then between the hemostats, with the bovie cuts through the vessel. Later we will return to each side of the cut and manually tie them off before releasing the hemostats. In one of the pictures you will see many hemostats exiting the wound, each stemming the blood flow from a vessel. I am caught by the visual; it is a circular ring of so many clamps that it strikes me more as the petals of a flower emanating from the opening we have made in this woman’s neck. So many in fact that when Mark asks for more, our table is out of them.
Finally, we are at the base of the goiter and it is ready to be removed with just a few more passes of the bovie. I have left the graphic and bloody images out that show me holding it in my hand after removal, but it is the size of a softball, and I am taken not only by its mass but how heavy it is. We are ready now to return to each of those many hemostats, and with a tie, cinch up and close off the end of the vessel. There is a bit of a choreograph to this. I lift the handle of the hemostat so it is almost vertical and Mark can pass the suture tie behind it, then I lower it so the curved tip of the hemostat is pointing up, so that he can bring the tie around fully to the front where he will create his surgeons knot under the tip. Having done this thousands of times, his fingers fly through motions so fast that I really could not duplicate the knot though I watched many many of them being tied during this trip. When done, I release and back the hemostats away from the knot and with my other hand come in with scissors to cut the tied legs short; he has already pulled both legs of the remaining material together and to the side so I can get at them with one snip. We repeat the process over and over and over until all hemostats are unclipped and all blood vessels tied off… then with a quick touch of the bipolar bovie that looks like forceps with two tips, Mark cauterizes and permanently finishes the complete closure of each. Two hours have passed. My back, arms, neck feel like I have just had a workout at the gym… and I wasn’t even doing the talented part of the process. Now we need to close the patient up so that things can heal rapidly, working from suturing the deepest tissues, to the final sutures just under the skin, that if done well you do not even see them on the skin surface of the neck. I had been practicing this at home before the trip, and I feel like I am ready for things……..
While not previously credited, I would like to thank the fastest learning photography student I have ever had for the fantastic images she captured that I and Mark are in. Carol D. Riggenbach (aka “grasshopper”).